 Importantly, side effects tend to occur more frequently at higher fluences and in darker-skinned individuals. A higher fluence may be used if a target is located deep within the skin or the chromophores are inefficient at absorbing light. IPL can deliver a fluence up to 40 J/cm^2, while pigmented lesions are usually treated with a fluence of only 16–20 J/cm2. Larger chromophores, such as hair follicles, require more time to cool down due to longer TRT.įluence (J/cm2) describes the amount of energy delivered per unit area. 
Delay times between sequential pulses are routinely 10 to 12 ms to accommodate epidermal TRT, whereas a 20-40 ms TRT is advised for patients with darker skin types. Thermal relaxation time is also adjusted to account for chromophore and lesion size. Allowing appropriate TRT between pulses also prevents epidermal temperatures from rising above 70 degrees C. Some IPL devices can only produce a single pulse, while others can produce multiple sequential pulses. 
To minimize thermal damage to the target tissue, the pulse duration should be shorter than its TRT. If the target is heated for a longer period than the TRT, the surrounding tissue may be impacted with subsequent scarring or hypopigmentation. Pulse duration is based on the thermal relaxation time (TRT) of the chromophore, or the time required for the temperature in a heated tissue to decrease to 37% of its peak. Given this same principle, shorter wavelengths effectively treat pigmented lesions in patients with lighter skin. Since melanin tends to absorb light at shorter wavelengths, selecting longer wavelengths that penetrate deeper and spare the epidermis may benefit darker skin patients. This concept is particularly important when administering IPL in patients with darker skin types, as special attention must be given to treat them safely and prevent dyschromias. For example, melanin in the epidermis may shield the targeted chromophores located in a deep layer of the skin. The skin contains different chromophores, molecules that absorb light of a specific wavelength and convert it to thermal energy. When selecting a wavelength, the healthcare provider should be aware of competing chromophores within the treatment area. The wavelength of light can be adjusted using cut-off filters, which allow certain tissues to be targeted via selective photothermolysis. The underlying mechanism of IPL therapy involves four crucial concepts (wavelength, pulse duration, fluence, and spot size):įlashlamps emit polychromatic light within a wavelength spectrum of approximately 400 to 1400 nm. This phenomenon of selective photothermolysis is the underlying basis of IPL technology. Chromophores (e.g., hemoglobin, water, melanin) in the skin absorb the photons and are subsequently heated by thermal energy, causing their destruction through thermocoagulation. Lasers and light devices produce a clinical effect when their light is absorbed by the skin, resulting in the emission of photons that carry thermal energy. Furthermore, the wavelength of light emitted from an IPL machine can be adjusted by applying filters. The advantage of broadband light is that it allows for greater versatility in treating a variety of skin types and conditions. IPL uses a flashlamp to emit polychromatic light across a broad wavelength spectrum of approximately 400–1400 nm, which makes it fundamentally different from a laser (light amplification by stimulated emission of radiation), whose light is necessarily monochromatic (of a single wavelength), collimated (with waves running in parallel), and coherent (with waves in phase). Currently, IPL is an invaluable tool in dermatology and is frequently used to address a broad range of medical and cosmetic concerns. IPL is safe and effective in treating benign pigmented and vascular disorders and hair removal and photoaging. 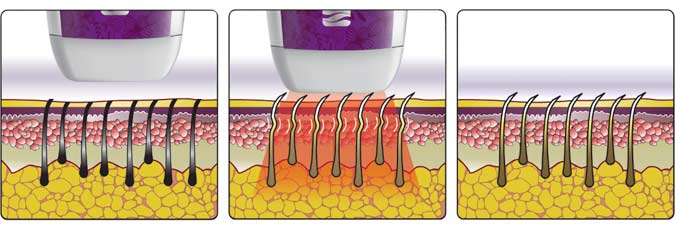
IPL devices are unique in that they employ flashlamps and bandpass filters to produce pulsed light of varying wavelengths, durations, and fluences. These aspects promote its versatility in treating numerous dermatological diseases. Since the first FDA-approved IPL device was brought to the market in 1995, this technology has undergone significant innovation and improvement in its clinical applications and affordability. Proof-of-concept studies were conducted on rabbit ear veins, demonstrating IPL's ability to thermocoagulate vessels while minimizing purpura or epidermal damage. Goldman, Fitzpatrick, and Eckhouse for the treatment of leg telangiectasias. Intense pulsed light (IPL) therapy was first developed in 1992 by Drs. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
